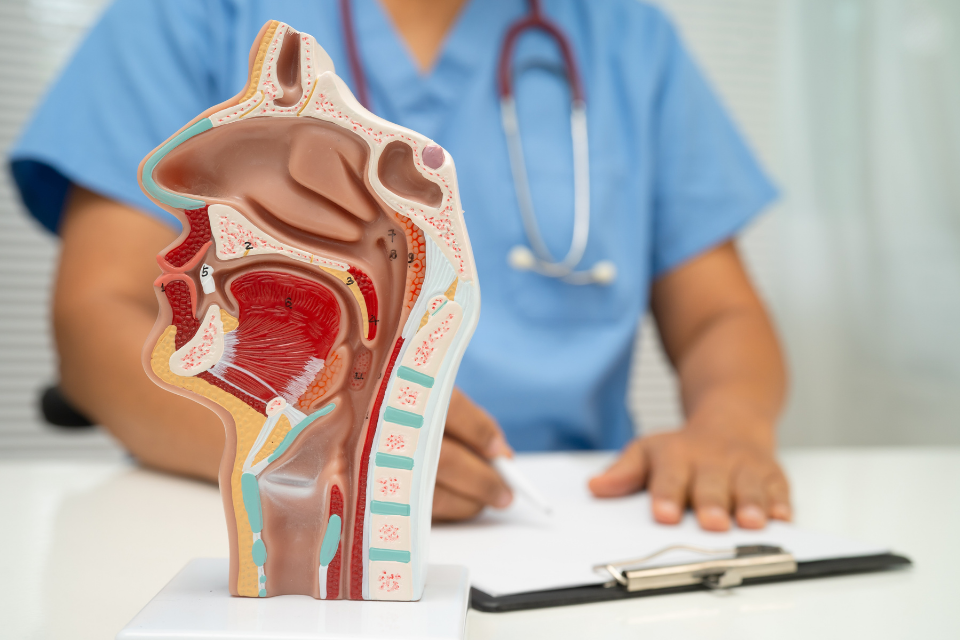
How to Stop Postnasal Drip: Causes and Effective Treatments
You know the feeling. That constant trickle in the back of your throat that makes you clear your throat in meetings, cough through dinner, and lie awake at 2 a.m. wondering if it's ever going to stop. Post nasal drip is one of the most common complaints ENT doctors hear — and one of the most frustrating to live with.
Here's what's actually happening: your nose and sinuses produce about 1–2 quarts of mucus every day. Normally, you swallow it without noticing. But when something triggers excess production or thickens that mucus, it starts pooling in your throat instead of moving along quietly. The result is that persistent drip, the scratchy throat, the cough that won't quit.
The good news is that figuring out how to stop post nasal drip starts with understanding what's causing it. This article breaks down the most common triggers, home remedies worth trying first, medical treatments for stubborn cases, and when it's time to see a specialist at Michigan Nose & Sinus Health.
What causes post nasal drip?
Post nasal drip isn't a condition on its own — it's a symptom. And the treatment that works depends entirely on what's driving it.
Allergies are the most common trigger. Pollen, dust mites, pet dander, and mold all provoke an inflammatory response in the nasal lining, ramping up mucus production. For Michigan residents, spring pollen season and fall mold counts make this a recurring problem. If your symptoms follow a seasonal pattern or flare up around pets, allergies and sinus inflammation are the likely culprit.
Sinus infections are another frequent cause. Acute sinusitis from a cold usually resolves in a week or two, but chronic sinusitis — defined as inflammation lasting 12 weeks or longer — can produce thick, discolored mucus and facial pressure that won't let up. This is one of the most common reasons post nasal drip becomes a long-term problem.
Acid reflux, specifically laryngopharyngeal reflux (LPR), is an often-overlooked cause. Stomach acid reaches the throat and nasal passages, creating a mucus sensation and constant throat clearing — frequently without any heartburn at all. Many patients don't connect their throat symptoms to reflux until an ENT evaluates them.
Structural issues like a deviated septum or enlarged turbinates can physically block drainage, trapping mucus in the sinuses. Other common causes include the common cold, cold dry Michigan winters, certain medications (blood pressure drugs, birth control), pregnancy, and spicy foods.
Home remedies and OTC treatments to try first
Many cases of post nasal drip respond well to simple at-home steps. These are worth a few weeks of consistent effort before moving to prescription options.
Stay hydrated and use saline rinses
Thin mucus clears easily. Thick mucus lingers. Drinking water, warm broth, and herbal tea throughout the day keeps mucus moving. Avoid overdoing caffeine and alcohol — both can dehydrate you and make things worse.
A saline nasal rinse is one of the most effective tools you can use at home. A neti pot or squeeze bottle flushes mucus and irritants directly from the nasal passages, and it's safe to do once or twice daily. Use distilled or previously boiled water only — never straight tap water.
Add moisture to your air
Dry indoor air — especially during Michigan's long winters — thickens mucus and irritates nasal tissue. A humidifier set to 40–50% humidity can make a real difference. Clean it regularly, though. A dirty humidifier breeds mold, which only makes the problem worse.
OTC medications
Steroid nasal sprays like fluticasone and budesonide reduce inflammation and work best with daily use, not as-needed. Antihistamines help when allergies are the cause — stick with second-generation options like loratadine or cetirizine, since older antihistamines can actually thicken mucus. Decongestant sprays offer short-term relief, but don't use them longer than three days or you risk rebound congestion.
Elevate your head at night
Sleeping propped up lets mucus drain forward rather than pooling in your throat. This alone can reduce the nighttime coughing and post nasal drip at night that keeps so many patients awake.
Post nasal drip vs. something else: symptoms that overlap
Post nasal drip shares symptoms with several other conditions, and mixing them up means the wrong treatment. Here's how to tell them apart:
Post nasal drip typically shows up as mucus in the throat (thin or thick depending on the cause), frequent throat clearing and coughing, and possible bad breath. You may notice reduced smell if nasal congestion is present, but you won't have heartburn and antacids won't help.
Acid reflux (LPR) creates a sensation of mucus in the throat, but there's often minimal actual drainage. Throat clearing and coughing are frequent. Heartburn may or may not be present — that's why it's called "silent reflux." The tell: symptoms respond to antacids and dietary changes.
Chronic sinusitis produces thick, discolored mucus along with facial pressure or pain, bad breath, and reduced sense of smell. A post nasal drip cough may be present, but the facial symptoms and persistent congestion are what set it apart.
The catch is that these conditions overlap. A patient can have allergies driving post nasal drip AND reflux making the throat symptoms worse at the same time. A post nasal drip sore throat doesn't automatically tell you which condition is responsible. That's exactly why an ENT evaluation can sort out what's actually going on — and point treatment in the right direction.
When home remedies aren't enough: medical treatments for post nasal drip
If you've been consistent with OTC options for 2–4 weeks and nothing's changed, it's time for a more targeted approach.
Prescription nasal sprays
Ipratropium (Atrovent) nasal spray specifically reduces mucus production — it's a different mechanism than steroid sprays and works well for patients with constant drainage. Prescription-strength steroid sprays are another option when over-the-counter versions aren't cutting it for persistent inflammation.
Allergy testing and immunotherapy
Guessing at your triggers wastes time. Allergy testing identifies exactly what's setting off your immune system so treatment can be precise. For long-term control, allergy drops (sublingual immunotherapy) or shots address the root cause of post nasal drip from allergies rather than just masking symptoms season after season.
Treating acid reflux and LPR
Dietary changes come first — no eating within three hours of bedtime, and cut back on acidic and spicy foods. When lifestyle changes fall short, proton pump inhibitors or H2 blockers can help. Expect 2–3 months of consistent treatment before judging results. LPR is slow to improve, and many patients give up too early.
Treating structural problems
A significantly deviated septum blocking drainage may need septoplasty. Turbinate reduction opens narrowed nasal passages. And for chronic sinusitis that hasn't responded to medication, balloon sinuplasty or endoscopic sinus surgery can restore proper sinus drainage.
The right post nasal drip treatment depends on an accurate diagnosis — which is why guessing only gets you so far.
When to see an ENT for post nasal drip
See an ENT if you're dealing with symptoms lasting longer than 10 days without improvement, thick green or foul-smelling mucus, facial pain or pressure alongside the drip, recurring sinus infections (three or more per year), a persistent cough that disrupts sleep or daily life, blood in your nasal mucus, or one-sided nasal symptoms like blockage or drainage from only one nostril. If your symptoms keep returning despite OTC treatment, that's another clear signal.
What happens at your ENT visit
Dr. Ulrich starts with a detailed exam of your nose, throat, and sinuses. A nasal endoscopy — a small camera placed into the nasal passages — lets him look directly at the internal structures and identify polyps, signs of chronic rhinitis, or areas of chronic infection that wouldn't show up otherwise. If allergies are suspected, testing can pinpoint your specific triggers. From there, you get a treatment plan built around what's actually causing YOUR symptoms — not a generic recommendation.
Finding lasting relief from post nasal drip
Post nasal drip is one of the most common reasons patients walk into an ENT office — and one of the most treatable once you know what's behind it. Allergies, sinus infections, reflux, and structural issues each call for a different approach, and that's exactly why the cause matters more than the symptom.
Home remedies like saline rinses and humidifiers are a reasonable starting point. But when symptoms persist beyond a few weeks, a specialist can identify what's going on and move you toward targeted solutions — from prescription sprays to in-office procedures.
If post nasal drip is disrupting your sleep, your daily routine, or your comfort, schedule an appointment with Dr. Ulrich at Michigan Nose & Sinus Health in Grand Blanc. Relief starts with finding the cause.
Frequently asked questions about post nasal drip
Can post nasal drip go away on its own?
It can, if the cause is temporary — a cold, a brief exposure to an irritant, or a short allergy flare. But post nasal drip lasting more than 10 days, or symptoms that keep coming back, usually need targeted treatment to fully resolve. Waiting it out rarely works for chronic cases.
Why is my post nasal drip worse at night?
Lying flat allows mucus to pool in the throat instead of draining forward through the nose. Dry bedroom air and allergens trapped in bedding make it worse. Sleeping with your head elevated and running a humidifier are two simple fixes that often reduce nighttime symptoms.
Can acid reflux cause post nasal drip?
Yes. Laryngopharyngeal reflux (LPR) irritates the throat and nasal passages, producing a mucus sensation and constant throat clearing — often without any heartburn. It's one of the most commonly missed causes, and treatment typically requires 2–3 months of dietary changes and medication before symptoms improve.